
Diabetes - Cause, Prevention, Treatment and Reversal with a Plant Based Diet
Summary
This is a long article, so here's the summary:
- In the next 25 years 1 in every 3 Americans will have developed type 2 diabetes.
- Type 2 diabetes is a serious progressive disease.
- Type 2 diabetes is largely a lifestyle-related disease and is preventable.
- Caused by diets high in saturated fat, not high in carbohydrates.
- Animal products and processed foods contain the vast majority of saturated fat in our diets.
- The excess fat inhibits insulin's effect so blood sugar levels remain dangerously high.
- By following a low-fat plant-based diet your risk of developing diabetes is very, very low.
- People with diabetes are at high risk for heart disease and stroke.
- Removing animal products from your diet helps lower your risk of having a heart attack or stroke.
- A low-fat plant-based diet has been proven to treat and reverse diabetes.
- Heart disease risk is also lowered by following a low-fat plant-based diet.
- A plant-based diet has been shown to work better than American Diabetes Association's guidelines in treating diabetes.
- Patients switching to a vegan diet didn't find it any harder to stick to than the ADA's recommended guidelines.
Diabetes will affect 1 in every 3 of us
Introduction
There are two forms of diabetes. Type 1 and type 2.
Type 1 diabetes is an autoimmune condition with the exact cause is currently unknown. It is partly inherited with multiple genes influencing the overall risk. Type 1 diabetes means the body doesn't produce insulin on it's own so insulin injections are required. There is currently no known way to prevent type 1 diabetes, but this form of diabetes only accounts for 5–10% of all cases of diabetes.[1]
However type 2 diabetes is far more common. This form of diabetes accounts for 90-95% of all diabetes cases, and is characterised by insulin resistance. Type 2 diabetes is a lifestyle related disease and as such is completely avoidable.
This article will discuss type 2 diabetes, which affects approximately 422 million people worldwide[2]. As the disease is preventable much more education is required to reduce the increasing prevalence, particularly amongst middle- and low-income countries.[3]
In the United States in 2011–2012, around 13% of adults had type 2 diabetes and 38% had pre-diabetes.[4]
Pre-diabetes means blood sugar level is higher than it should be, but not yet high enough to be classed as type 2 diabetes (the blood sugar is borderline high). It's an early indicator of growing insulin resistance, and without lifestyle changes, people with pre-diabetes are very likely to progress to type 2 diabetes.
Interestingly, even before the development of pre-diabetes, the insulin resistance (IR) score becomes elevated, which is a herald of bad news, indicating high blood glucose levels are right around the corner. So here’s the sequence of events:
Abnormal lipid levels (reversible)→ Insulin resistance (reversible) → Pre-diabetes (reversible) → Diabetes type 2 (may be reversible in early stages before the pancreas fully burns out)→ Advanced diabetes (irreversible) with end organ damage (kidney failure, heart disease, nerve damage, and blindness, etc ). Please note that reversible in parenthesis indicates the possibility of reversing disease through dietary or life-style changes.
Prediabetes is very common in those aged over 65 in the United States affecting over 50% of people in this age bracket.[5]
Because the early symptoms of type 2 diabetes are mild, the disease isn't taken as seriously as it should be. That’s why diabetes is a silent killer. Early symptoms include increased thirst, frequent urination, and unexplained weight loss. However pre-diabetes is completely asymptomatic and the only way to diagnose pre-diabetes is through a blood test.
However the disease is progressive and is the 7th leading cause of death in the United States, which develops more severe symptoms including increased risk of overall mortality, reduced quality of life and increased risk of institutionalization. Older patients also have the highest rates of additional complications from diabetes, including heart attacks, stroke, amputations, end-stage kidney disease, and visual impairment eventually leading to blindness.
The British National Health Service reports that diabetes is a leading cause of amputation - most often feet/toes - and states people with diabetes are 15 times more likely[6] to undergo amputations than other people without the condition. In fact, in the UK more than 140 diabetes-related amputations occur every week[7] - a record 21,125 diabetes-related amputations were completed between 2011 and 2014 in England - seven more a week than the three previous years[8]. Other symptoms include failing eyesight leading to blindness.
Because diabetes is so common, with severe consequences including a sudden cardiac death due to a massive heart attack, and the fact that it is entirely preventable (and reversible) proper diagnosis and education is key to help reduce this disease. Currently, due to traditional old fashion testing (Basic lipid panel, fasting blood sugar, HbA1c), the disease is underdiagnosed, therefore undertreated. Modern tests for Insulin Resistant score and LDL sub particles are able to detect the early stages of disease and provide and opportunity for patients to intervene and reverse disease.
How about starting a cholesterol medicine (statin) for elevated cholesterol levels to possibly prevent diabetes? Unfortunately that doesn’t work very well. In the Women’s Health Initiative Trial, which included 153,840 post menopausal patients without diabetes, statin therapy was associated with an increased risk of new-onset diabetes. Other studies have confirmed these findings. So is it worth treating the elevated cholesterol levels with a statin drug to reduce the risk of heart disease and induce diabetes? Unfortunately this happens more often than you think. Patients with high cholesterol levels are treated with statin drugs, without attention to elevated Insulin Resistance score, and as a result develop full blown diabetes. The mechanism of action is most likely related to down regulation of the insulin transporter. Fortunately, there is a solution. Although drugs are ineffective and harmful in this case scenario, a whole plant based diet and weight loss (losing as little as 10% of body fat) has shown to reverse disease.
Cause
The cause of diabetes is commonly believed to be "too much sugar", however this is not the cause, but a symptom.
Dr. Angie Sadeghi explains type 2 diabetes
Studies dating back to 1927[9] noted a interesting finding.
Young, healthy people were taken and split into two groups — half on a fat-rich diet and half on a carbohydrate-rich diet — and within just two days, glucose intolerance skyrocketed in the fat group. The group on the fat-rich diet ended up with twice the blood sugar. And as the amount of dietary fat increased, so did the blood sugar. But it took scientists nearly seven decades to unravel the mystery of why fat causes type 2 diabetes.
Why does fat cause type 2 diabetes?
When food is consumed, starches are broken down into glucose in our digestive system, it then circulates as blood glucose ("blood sugar") and is taken up by our muscles to either be stored (as glycogen) or burnt and used for energy.
Insulin acts as a 'key' to unlock the door and let glucose enter the muscle cells. Without insulin, glucose would remain in the blood, steadily rising to a state called hyperglycemia - high blood sugar. With Type 1 diabetes, the cells in the pancreas that produce insulin are damaged so cannot produce insulin, and so insulin injections are required in order for the glucose to move out of the blood into the muscles.
However in type 2 diabetes normal insulin exists - but the insulin is unable to 'unlock' the muscle cells so the sugar cannot enter the muscle cells and remains in the blood, again leading to dangerously high levels of blood sugar.
So why can't the insulin unlock the muscle cell to let the sugar in? Tiny droplets of fat inside our muscle cells known as intramyocellular lipids block the pathway into the muscle cells preventing the glucose from entering.
Fat in the bloodstream builds up inside the muscle cells creating toxic fatty breakdown products and free radicals that block the insulin signaling process.
No matter how much insulin we have in our blood, it’s not able to sufficiently open the glucose gates, and blood sugar levels build up in the blood. And this can happen within three hours[10]. Studies have shown that one hit of fat can start causing insulin resistance, inhibiting blood sugar uptake after just 160 minutes.
This mechanism by which fat causes insulin resistance wasn’t clear until MRI techniques were developed[11] to see exactly what was happening inside people’s muscles as fat was infused into their bloodstream. That’s how we found that elevation of fat levels in the blood causes insulin resistance by inhibition of glucose transport into the muscles.
Dr. Michael Greger explains type 2 diabetes
The opposite is also true - when the level of fat in people's blood is lowered, the insulin resistance comes back down again[12].
This is one of the reasons why a high-fat ketogenic style diet is unhealthy - it causes insulin resistance. As the level of fat in our diet lowers, insulin works better and better.
After comparing diets and diabetes rates in different countries we know that as carbohydrate intake goes down and fat intake goes up, the number of diabetics rapidly increases[13]. And the difference is not down to genetics, because we have seen when people move to countries where the standard ‘Western’ style diet predominates and they adopt this diet, their rates of type 2 diabetes increase above the national average[14].
Further research has suggested that eating just one serving of meat per week significantly increases the risk of diabetes. A study looked at the link between meat intake and the occurrence of diabetes in 8,000 adult Seventh Day Adventists, all of whom were non-diabetic at the start of the study[15]. It showed those who followed a ‘low-meat’ diet over the 17 years of this long-term study had a staggering 74% increase in their risk of developing type 2 diabetes compared to participants who followed a meat-free diet for the same period.
Some of the difference was attributable to obesity and/or weight gain but even after allowances were made for this, meat intake still remained an significant risk factor in developing diabetes.
Another study published in 2004 produced a remarkable discovery[16] and confirmed the findings of previous studies[17]. The researchers tested young healthy adults, whose family members were diabetic, for insulin resistance. Those who tested positive were found to have microscopic drops of fat in their muscle cells. This fat interfered with the cells’ ability to correctly react to insulin. Even though their bodies produced sufficient insulin, fat inside their cells inhibited the correct reactions.
But what about carbohydrates?
Studies have shown that carbohydrates can reduce diabetes. An experiment was setup to compare high-protein diets with high-carbohydrate diets with patients with type 2 diabetes. They were split into two groups - the high-carbohydrate group was instructed to eat more bread, cereal, pasta, and starchy vegetables while the high-protein group was instructed to have more fish, chicken, eggs, low fat milk, cheese, and nuts. The experiment was ran over a period of 8 weeks and their fat intake was kept constant at 30%. Both groups experienced equivalent weight-loss, but the diabetes improved (blood sugar control improved) in only the carbohydrate group.
Low carbohydrate diets have also been found to actually increase the risk of type 2 diabetes - a study found a 37% increase in risk of diabetes. Interestingly, several studies have also shown that low-carbohydrate diets based on animal sources carry an increased risk of developing diabetes whilst low carbohydrate plant-based diets prove protective.[18][19][20]
Several studies have also associated low-carbohydrate diets with increased all-cause, cardiovascular, and cancer mortality.[21][22][23][24]
Treatment
Treatment is either drugs or lifestyle changes. Drugs come with a myriad of side effects, and could possibly worsen the disease state, but lifestyle changes have shown to be highly effective. In particular, a whole food plant-based diet, devoid of dairy and meat, low in saturated animal fat, has consistently been shown to be a highly effective treatment. A whole food plant based diet enables people with diabetes, high cholesterol, and heart disease to reverse diabetes and possibly discontinue medications.
Studies have shown that some drugs lower blood sugar but at the same time can increase the chances of heart attacks and strokes, or come with other adverse side effects.[25]
The Academy of Nutrition and Dietetics, the largest organisation of dieticians in the world, states that:
"Vegetarian and vegan diets are appropriate for all stages of life, from infancy to adulthood, and may provide benefits for the prevention and treatment of diabetes, obesity and ischemic heart disease."
And they're not wrong - dozens of studies have now shown the effectiveness of a plant-based diet to prevent and treat diabetes.
Using a plant-based diet to control diabetes also comes with the added bonus of lowering the risk for heart disease, cancer, obesity, strokes and hypertension.
As far back as the 1950s, studies have been published on treating diabetes with a high-carbohydrate, low-fat diet,[26][27][28] documenting the effectiveness of employing a predominantly vegetarian diet to treat diabetes. Barnard et al.,[29] performed the first major randomized clinical trial on diabetic patients treated purely with a plant-based (vegan) diet, comparing it to a conventional diet based on the 2003 American Diabetes Association (ADA) guidelines.
A total of 99 individuals, ages 27–82 years, were randomized to follow either a low-fat vegan diet or the ADA diet and tracked for 22 weeks. The recommended vegan diet comprised approximately 10% of energy from fat, 15% from protein, and 75% from carbohydrates and consisted of vegetables, fruits, grains, and legumes.
Participants in the vegan group were asked to avoid animal products and added fats and to favor low-glycemic index foods, such as beans and green vegetables. By the end of the trial, 43% (21 of 49) of the vegan group and 26% (13 of 50) of the ADA group participants reduced their diabetes medications. Excluding those who changed medications, hemoglobin A1c fell 1.23 points in the vegan group compared with 0.38 points in the ADA group. Body weight decreased 6.5 kg in the vegan group and 3.1 kg in the ADA group.
LDL cholesterol also fell 21.2% in the vegan group and 10.7% in the ADA group, reducing the risk of a heart attack.
But did the diabetes get better just because of weight loss?
High-carbohydrate low-fat (HCLF) plant-based diets are associated with weight-loss, and weight-loss is associated with an improvement in diabetes - but was it the weight-loss alone that caused the improvement in diabetes, or was it the plant-based diet?
In 1979 another experiment[30] was conducted where patients were weighed every day - and if they started losing weight they were made to eat more food so they had no significant weight loss. Even with no weight-loss, overall insulin requirements were reduced by about 60%, and half of the diabetics were able to stop taking their insulin altogether in just 16 days on a plant-based diet. Some diabetics who had been taking insulin for 20 years, and injecting 20 units of insulin a day were off insulin altogether in as few as 13 days after cutting out all animal products and adopting a plant-based diet.
This chart from the experiment shows patient #15 who was injecting 32 units of insulin on the control diet, and then, 18 days later is able to stop taking insulin with lower blood sugars than when he was on insulin.
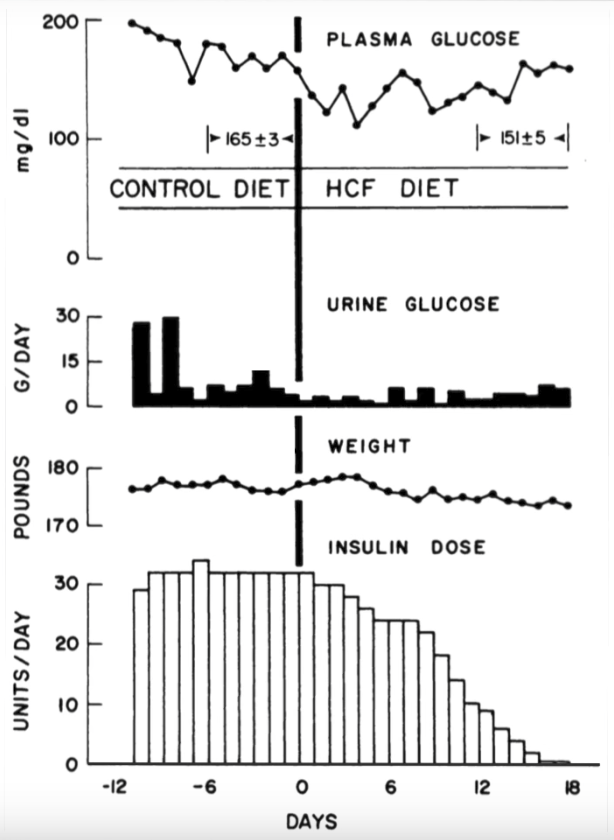
From the experiment patient #15 was injecting 32 units of insulin on the control diet, and then, 18 days later, on none. Lower blood sugars on 32 units less insulin.
And, as a bonus, their cholesterol dropped dramatically to under 150 — in just 16 days - also cutting their chance of a heart attack or stroke.
Discontinuing all medication
Another study in 1982 on a group of 40 type 2 diabetic patients had outstanding results – 36 of the patients were able to discontinue all medication after only 26 days[31]. A year later another study demonstrated that the benefits of this diet are long-term and last for years if the diet is continued. [32]
In 1994, another groundbreaking study followed when researchers employed a combination of diet change and exercise[33]. The subjects were 197 men with type 2 diabetes and after just three weeks of a low-fat plant-based diet, 140 of them were able to discontinue their medication.
But is sticking to a a vegan diet difficult?
Switching to a vegan diet might seem like it would be difficult for patients to stick to, however it's worth noting that even though the vegan diet required greater changes to be made than the ADA recommended diet, multiple studies[34][35][36] have shown there was no difference to the acceptability or adherence of the diet. While this may be surprising given the potential degree of change required to adopt a vegan diet, the authors hypothesized that not limiting portion sizes, not counting calories or carbohydrates, and experiencing of a variety of new flavors in the vegan diet likely offset any hardship imposed by restricting animal products or added oils.
How do plant-based diets help reverse diabetes?
There are a variety of ways that plant-based diets are thought to improve blood sugar control.
Plant-based diets tend to be low in saturated fat, which as we described earlier, contributes to lipotoxicity - impairing the insulin signalling in liver and muscle cells and decreasing glucose uptake from the bloodstream.
But it doesn't end there.
Plant-based diets are high in fiber, antioxidants and magnesium, all of which have been separately shown to improve insulin sensitivity.[37][38]
Additionally, the gut bacteria of vegans produces substantially less trimethylamine N-oxide (TMAO), a compound that has been tied to insulin resistance[38][40][41], as well as increased risk of atherosclerosis[42][43].
Plant based diets are also much lower in other dietary elements associated with insulin resistance such as advanced glycation end products, nitrosamines and heme iron. Many of these dietary elements additionally increase the risk of heart disease, which, as previously mentioned, is already higher for diabetics.
Blood sugar can decrease relatively quickly
Diabetics who switch to a plant-based diet can experience decreases in blood sugar and blood pressure relatively quickly after changing their diet, especially if they are taking medications for these conditions, therefore close monitoring and anticipation of low blood sugar is critical, as medications may require lowering or ceasing altogether to avoid blood sugar becoming too low (hypoglycemia). [44]
Dr. Michael Greger summarizes diabetes prevention, treatment and reversal
The Future
Many organisations are now seeing the benefits of using plant-based diets for preventing and treating diabetes and other related diseases.
Large healthcare organizations such as Kaiser Permanente are promoting plant-based diets for all of their patients and employees because it is a cost effective, low-risk method of treating numerous chronic illnesses simultaneously and is seen as an important tool to address the rising cost of health care.
The usefulness of vegan diets has even finally been endorsed by the American Diabetes Association in their 2010 Clinical Practice Guidelines which stated that "plant-based diets had been shown to improve metabolic control in persons with diabetes."
However the ADA receives heavy sponsorship from meat and dairy companies as well as pharmaceutical firms - as detailed in the 2017 documentary What The Health - so don't expect the ADA to advocate elimination of animal products or adoption of a plant-based diet for treatment/reversal while this situation continues.
Bizarre interview with Dr. Robert Ratner - Chief Scientific and Medical Officer at the ADA
Documentary What The Health exposes the link between the ADA and corporate sponsors
Legal disclaimer: The contents of this website, such as text, graphics, images, and other material contained on the website ("Content") are for informational purposes only and do not constitute medical advice; the Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of a physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
References
1. http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(06)68341-4/fulltext
2. http://www.who.int/mediacentre/factsheets/fs312/en/
3. World Health Organization Diabetes Fact Sheet. http://www.who.int/mediacentre/factsheets/fs312/en/ (accessed November 27, 2016).
4. Menke A, Casagrande S, Geiss L, et al. Prevalence of and trends in diabetes among adults in the united states, 1988–2012. JAMA 2015; 314: 1021–1029.
5. Caspersen CJ, Thomas GD, Boseman LA, et al. Aging, diabetes, and the public health system in the United States. Am J Public Health 2012; 102: 1482–1497.
6. http://www.diabetes.co.uk/diabetes-and-amputation.html
7. https://www.diabetes.org.uk/About_us/News/More-than-135-diabetes-amputations-every-week/
8. Public Health England data
9. http://jamanetwork.com/journals/jamainternalmedicine/article-abstract/535594
10. http://www.ncbi.nlm.nih.gov/pubmed/10334314
11. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC507380/
12. http://www.ncbi.nlm.nih.gov/pubmed/0010480616
13. Campbell & Campbell, 2004; Barnard, 2007
14. Tsunehara et al., 1990
15. Vang et al., 2008
16. Petersen et al., 2004
17. Phillips et al., 1996; Krssak et al., 1999
18. de Koning L, Fung TT, Liao X, et al. Low-carbohydrate diet scores and risk of type 2 diabetes in men. Am J Clin Nutr2011; 93: 844–850
19. Halton TL, Liu S, Manson JE, et al. Low-carbohydrate-diet score and risk of type 2 diabetes in women. Am J Clin Nutr2008; 87: 339–346
20. Bao W, Li S, Chavarro JE, et al. Low carbohydrate-diet scores and long-term risk of type 2 diabetes among women with a history of gestational diabetes mellitus: a prospective cohort study. Diabetes Care 2016; 39: 43–49
21. Sjogren P, Becker W, Warensjo E, et al. Mediterranean and carbohydrate-restricted diets and mortality among elderly men: a cohort study in Sweden. Am J Clin Nutr 2010; 92:967–974
22. Noto H, Goto A, Tsujimoto T, et al. Low-carbohydrate diets and all-cause mortality: a systematic review and meta analysis of observational studies. PLoS One 2013; 8: e55030.
23. Lagiou P, Sandin S, Lof M, et al. Low carbohydrate-high protein diet and incidence of cardiovascular diseases in Swedish women: prospective cohort study. BMJ 2012; 344:e4026
24. Fung TT, van Dam RM, Hankinson SE, et al. Low-carbohydrate diets and all-cause and cause-specific mortality:two cohort studies. Ann Intern Med 2010; 153: 289–298
25. https://www.nytimes.com/2017/06/05/health/type-2-diabetes-blood-sugar-heart-risk.html
26. Singh I. Low-fat diet and therapeutic doses of insulin in diabetes mellitus. Lancet 1955; 268: 422–425
27. Kempner W, Peschel RL, Schlayer C. Effect of rice diet on diabetes mellitus associated with vascular disease. PostgradMed 1958; 24: 359–371
28. Anderson JW, Ward K. High-carbohydrate, high-fiber diets for insulin-treated men with diabetes mellitus. Am J Clin Nutr1979; 32: 2312–2321
29. Barnard ND, Cohen J, Jenkins DJ, et al. A low-fat vegan diet improves glycemic control and cardiovascular risk factors in a randomized clinical trial in individuals with type 2 diabetes.Diabetes Care 2006; 29: 1777–1783
30. http://www.ncbi.nlm.nih.gov/pubmed/495550
31. Barnard et al., 1982
32. Barnard et al., 1983
33. Barnard et al., 1994
34. Barnard ND, Gloede L, Cohen J, et al. A low-fat vegan diet elicits greater macronutrient changes, but is comparable in adherence and acceptability, compared with a more conventional diabetes diet among individuals with type 2 diabetes. J Am Diet Assoc 2009; 109: 263–272
35. Ornish D, Scherwitz LW, Billings JH, et al. Intensive lifestyle changes for reversal of coronary heart disease.JAMA 1998; 280: 2001–2007
36. Turner-McGrievy GM, Barnard ND, Scialli AR. A two-year randomized weight loss trial comparing a vegan diet to amore moderate low-fat diet. Obesity (Silver Spring) 2007; 15:2276–2281
37. Ley SH, Hamdy O, Mohan V, et al. Prevention and management of type 2 diabetes: dietary components and nutritional strategies. Lancet 2014; 383: 1999–2007
38. Satija A, Bhupathiraju SN, Rimm EB, et al. Plant-based dietary patterns and incidence of type 2 diabetes in US men and women: results from three prospective cohort studies
39. Satija A, Bhupathiraju SN, Rimm EB, et al. Plant-based dietary patterns and incidence of type 2 diabetes in US men and women: results from three prospective cohort studies
40. Kim Y, Keogh J, Clifton P. A review of potential metabolicetiologies of the observed association between red meat consumption and development of type 2 diabetes mellitus.Metabolism 2015; 64: 768–779
41. Li D, Kirsop J, Tang WH. Listening to our gut: contribution of gut microbiota and cardiovascular risk in diabetes pathogenesis. Curr Diab Rep 2015; 15: 63
42. https://www.ncbi.nlm.nih.gov/pubmed/23563705
43. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3650111
44. Trapp C, Barnard N, Katcher H. A plant-based diet for type 2 diabetes: scientific support and practical strategies. DiabetesEduc 2010; 36: 33–48
Subscribe!
Love this content?
Receive our awesome newsletter straight to your Inbox!

 Your email address will always stay private.
Your email address will always stay private.
























Comments
Wish you had links to the referenced studies